Proposed cure for Hong Kong’s public health system will not give hospitals the lifeline they need, experts warn
As a rapidly ageing population further strains resources, experts accuse the government of not doing enough to tackle a chronic shortage of doctors
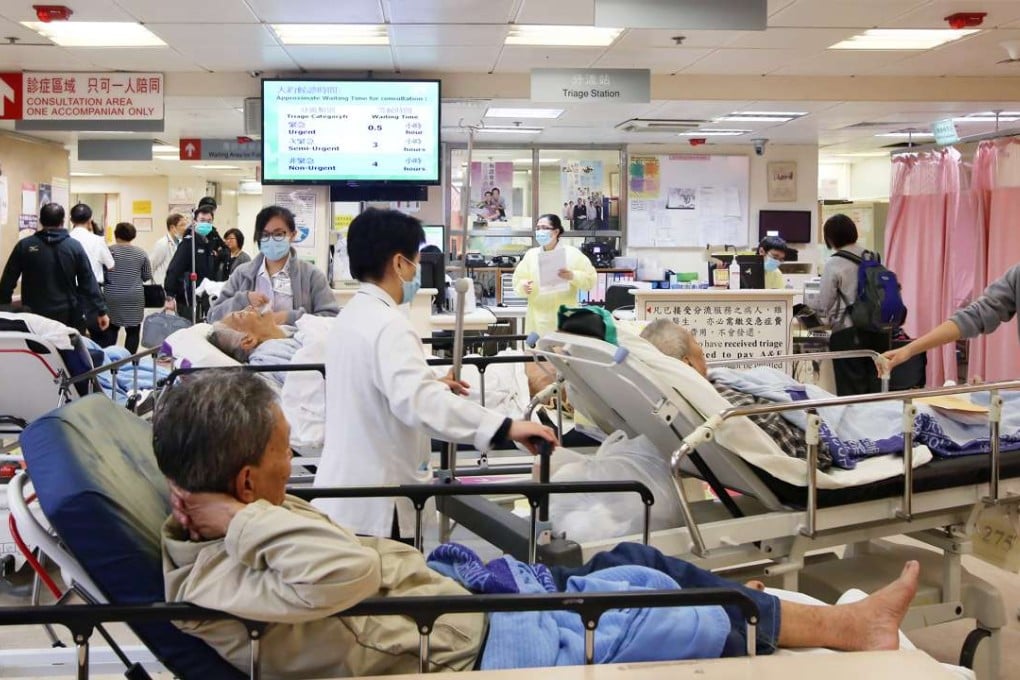
Medical experts warn that government plans to address the acute manpower shortage plaguing Hong Kong’s health system are unlikely to ease the pressure.
In recent years, public hospitals have faced a chronic shortage of about 300 doctors, leading to massive spikes in waiting times and a system that is often stretched to breaking point. The number of doctors needed is projected to increase by about 28 per cent from 6,310 in 2016 to 8,050 in 2026, according to a 2015 Food and Health Bureau report.
The city’s nurse-to-patient ratio is also behind the international standard of 1:6. The average ratio of nurses to patients in public hospitals was 1:11 but could reach 1:24 at night, the Association of Hong Kong Nursing Staff reported earlier this year.
The shortages are the result of many factors, including a lack of new doctors, stringent requirements for non-locally trained doctors to practise in the city, a lucrative private health sector, and an emphasis on secondary care such as specialist and hospital services over primary care like health promotion and prevention.