How to spot symptoms of colorectal cancer, the second most common cancer in Hong Kong
Many Hongkongers do not bother screening and ignore symptoms such as cramps and rectal bleeding, putting themselves at risk of this killer disease
Routine colon cancer screening has been proven to save lives, but people often avoid getting tested because of the unpleasant procedure.
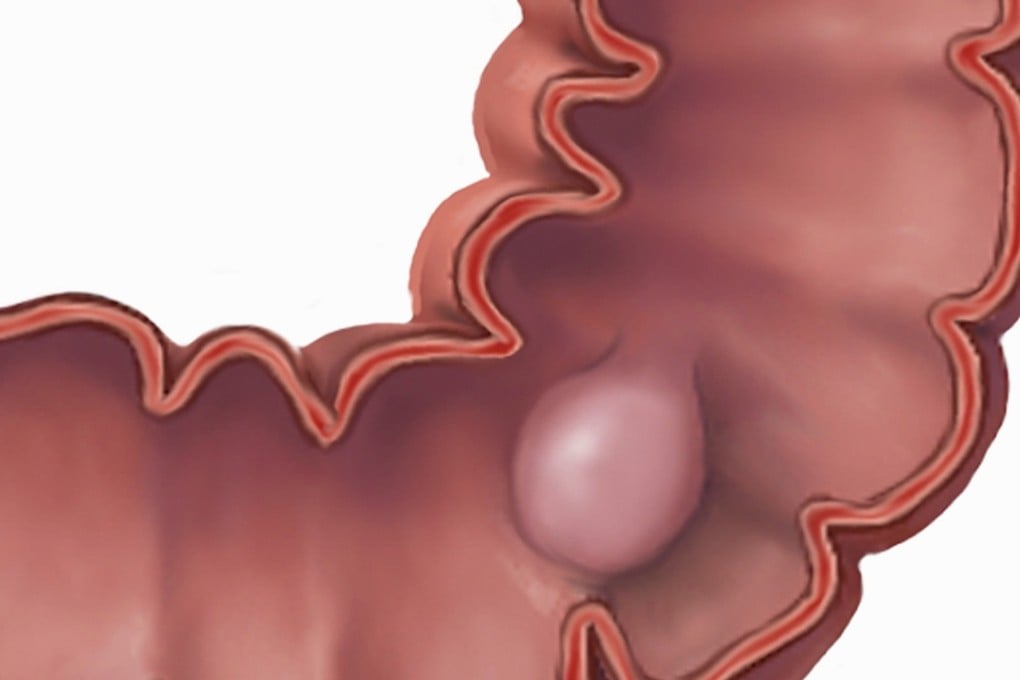
By snaking a camera through a patient’s intestines – a procedure called a colonoscopy – doctors can identify colon cancer in its infancy and remove the polyps and other abnormal growths before they eventually become cancerous.
There could soon be a less invasive and cheaper alternative screening method to the uncomfortable and invasive colonoscopy. It could induce encourage more people to get tested: a simple blood test.
Researchers at Canada’s BC Cancer Agency, collaborating Fujian Normal University scientists, have identified differences in the blood of people with precancerous polyps compared to people without such polyps. The researchers say the initial results are promising, but the procedure is still in the research phase and must go through additional lab tests and clinical trials before implementation.
For now, the other non-invasive colon cancer screening mechanism available is the faecal occult blood test, which looks for microscopic traces of blood in stool samples, a potential sign of cancer. However, many early-stage colon cancers are asymptomatic and don’t bleed, leaving them undetectable by this measure.