Experts fear return of Hong Kong’s No 1 killer, TB, amid rise in visitors from disease hot spots and drug resistance
Deaths from tuberculosis peaked in Hong Kong in 1951, but with an increase in antibiotic-resistant strains, more tourists from disease hot spots, and the city’s growing number of elderly, doctors fear a resurgence

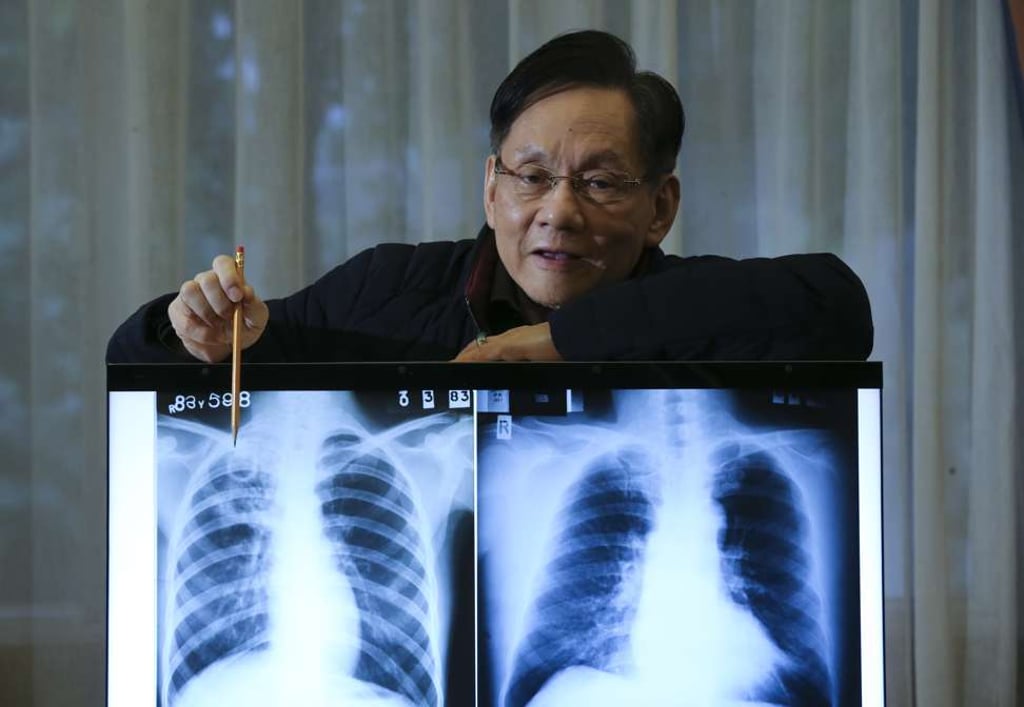
Dr Chan Shiu-lun is well qualified to identify the signs of tuberculosis from the chest X-ray of a young Hong Kong man, diagnosed with the deadly disease. The chest physician and honorary consultant to the Hong Kong Tuberculosis, Chest and Heart Disease Association, points to a distinctive white circular shadow, which he says is a cavity in the upper right section of the patient’s lung.
In Hong Kong, tuberculosis (TB) – also known as “consumption” or the “white plague” – was once the city’s biggest killer. In the decade after the second world war, when poor immigrant communities were often crowded into cramped, insanitary makeshift shacks, TB was rampant. Annual deaths from the disease were three times the number killed by the outbreak of severe acute respiratory syndrome (Sars) in 2002 and 2003. In 1951, fatalities peaked at 4,190 (or 208 for every 100,000 of the population), but these days it’s often dismissed as a nasty disease from the distant colonial era.
“TB is still with us and it’s still killing people,” says Chan.
A comprehensive report published in 2016 by the World Health Organisation (WHO) revealed TB to be one of the top 10 causes of death worldwide, claiming more lives than HIV or malaria. In 2015, 10.4 million people fell ill with TB and it claimed 1.8 million lives. According to the WHO, six high-TB- burden countries accounted for 60 per cent of the total, with India leading the count, followed by Indonesia and China.