Glaucoma explained, and why regular eye checks are vital for the over-40s
A group of eye diseases associated with optic nerve damage, glaucoma affects three per cent of the population. Sometimes symptom-free, it is often diagnosed too late, and the loss of vision cannot be reversed
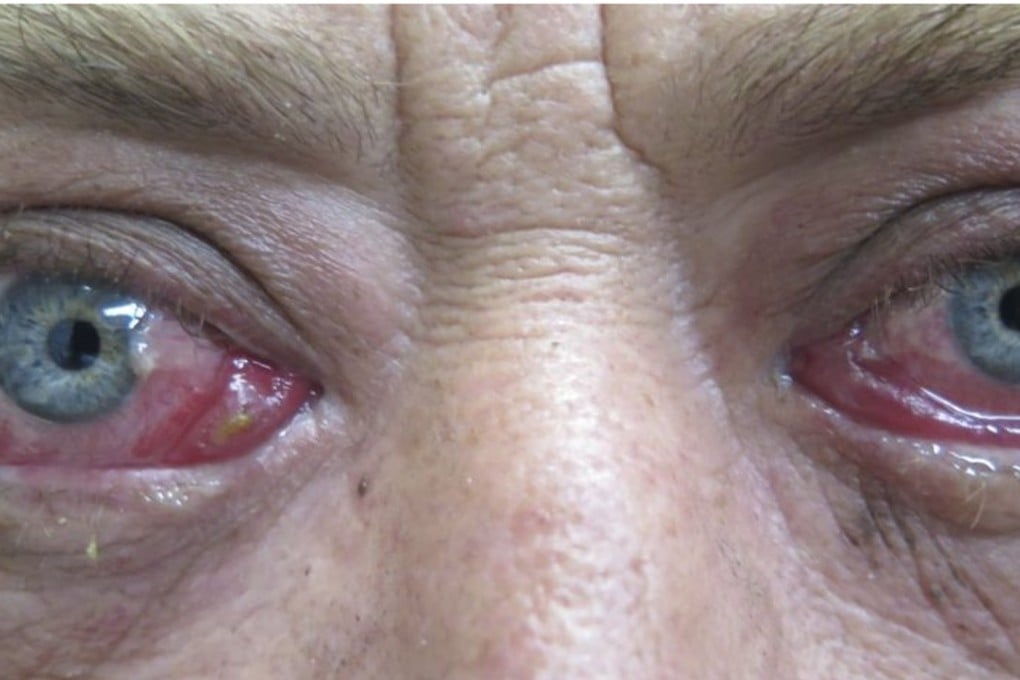
Newly diagnosed glaucoma sufferers are often shocked upon learning their failing eyesight cannot be restored to their original acuity, that there is no cure. If unchecked, victims can go blind.
Glaucoma is a group of eye diseases associated with the degeneration of the optic nerve that carries information from the eyes to the brain. This leading cause of irreversible blindness in the city affects three per cent of Hongkongers aged 40 or over, according to the Hospital Authority.
The chronic kind, “primary open angle glaucoma,” is most common and often asymptomatic. Victims may not notice their vision is eroding until much of it has gone.
It’s a myth, you won’t see better by eating fish eyes
Inside a healthy eye is a “rim” full of neural tissue; in a patient with glaucoma, that “rim” has thinned, disrupting the vision process. The cause is not fully understood.
“Even in normal people, you lose optic fibres everyday as part of the ageing process, but in glaucoma patients, the loss happens at a far higher rate than the average person,” says Tham.