Depression treatment: drugs, behavioural or electroconvulsive therapy – which works the best?
ECT has been used to treat depression and other mental illnesses for 80 years. A study suggests it may be more effective than previously thought, and comes at a time when views about using medication to treat depression are changing
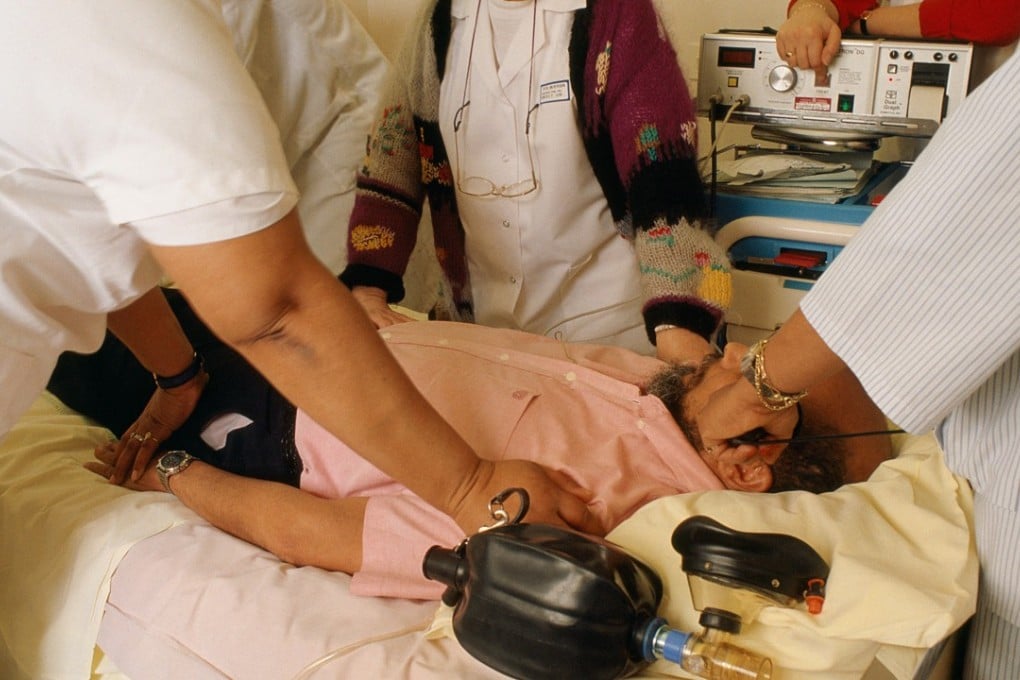
Eighty years ago at Sapienza University in Rome, Italy, doctors sent a jolt of 100 volts of electricity through the head of a man who had been diagnosed with schizophrenia. Within weeks, he appeared to be better and returned to work as an engineer.
He was the first patient to undergo what was then called ES and is now known as ECT – electroconvulsive therapy. Although his symptoms returned, the doctors knew they were treatable.
The treatment, which remains stigmatised after it was unfavourably depicted in Hollywood films (think One Flew Over the Cuckoo’s Nest), may be about to make a comeback, following a study that suggests it should be made be made available more often and sooner to people with severe depression.
Some suggest it works in 80 per cent of cases. But it is not a panacea; it comes with risks.
My mother was subjected to ECT back in the 1970s. It didn’t cure her. It shocked her back to wellness, briefly and, she says, affected her short-term memory – one of the side effects, along with headaches.
Today the treatment is much more gentle – mild, electrical impulses – and cost effective for what psychiatrists call “treatment resistant” depression which won’t budge after the administration of at least two other options – say drugs and therapy.