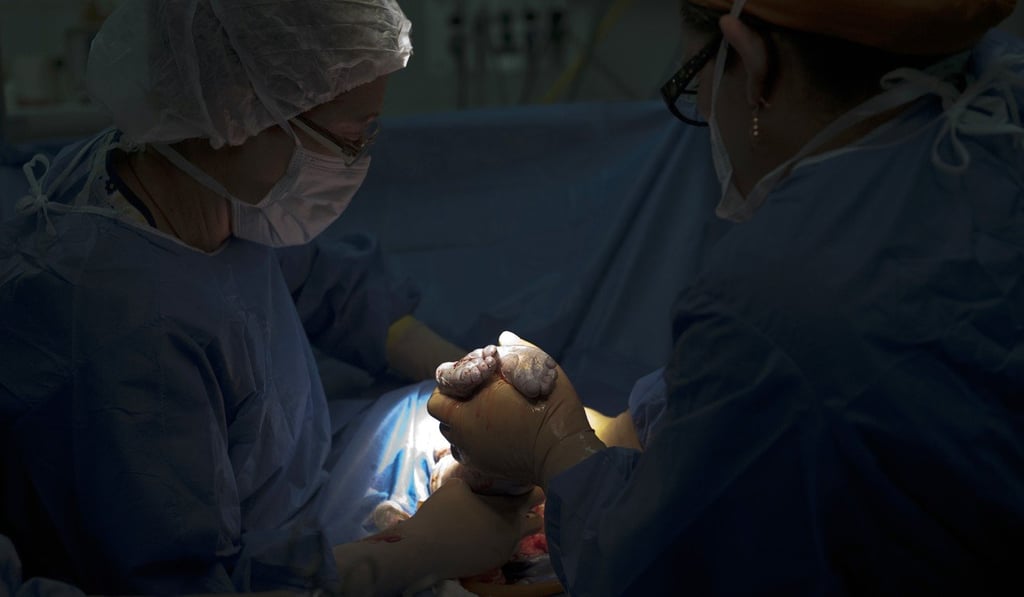
C-section study shows huge childbirth care gap between rich and poor mothers
New research on caesarean section procedures suggests rich mothers get too many while poor ones get too few, as doctors warn that number of procedures has reached ‘epidemic’ proportions in some countries
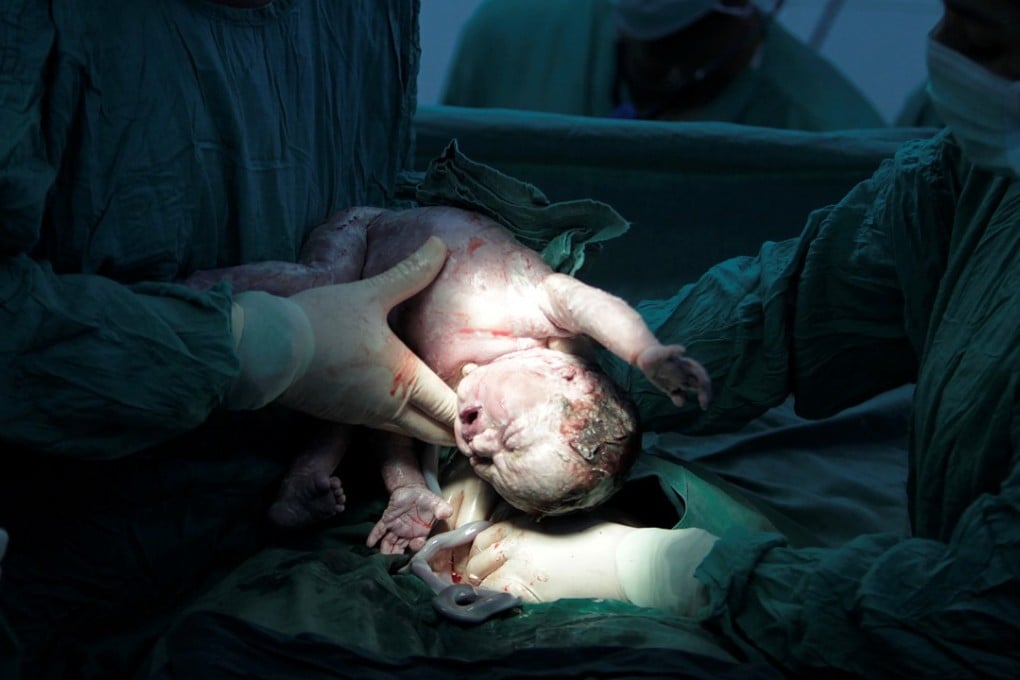
The number of babies delivered by caesarean section worldwide has nearly doubled in two decades and has reached “epidemic” proportions in some countries, doctors warned, highlighting a huge gap in childbirth care between rich and poor mothers.
They said millions of women each year may be putting themselves and their babies at unnecessary risk by undergoing C-sections at rates “that have virtually nothing to do with evidence-based medicine”.
In 2015, the most recent year for which complete data is available, doctors performed 29.7 million C-sections worldwide – 21 per cent of all births. This was up from 16 million in 2000, or 12 per cent of all births, according to research published in The Lancet. It is estimated that the operation – a vital surgical procedure when complications occur during birth – is necessary 10-15 per cent of the time.
But the research found wildly varying country rates of C-section use, often according to economic status: in at least 15 countries more than 40 per cent of births are performed using the practice, often on wealthier women in private facilities.
In Hong Kong, about 41 per cent of births are by C-section. In Brazil, Egypt and Turkey, more than half of all births are done via C-section. The Dominican Republic has the highest rate of any nation, with 58.1 per cent of all babies delivered using the procedure.