Advertisement
Medical staff suffering insomnia while treating coronavirus cases likely also to be depressed and anxious, research shows
- Frontline medical staff who regularly lost sleep during the peak of the pandemic in China are, according to a study, more likely to feel depressed and anxious
- Suggested strategies to overcome sleep disorders include stress relief to overcome negative thoughts and cognitive behavioural therapy for insomnia
Reading Time:2 minutes
Why you can trust SCMP
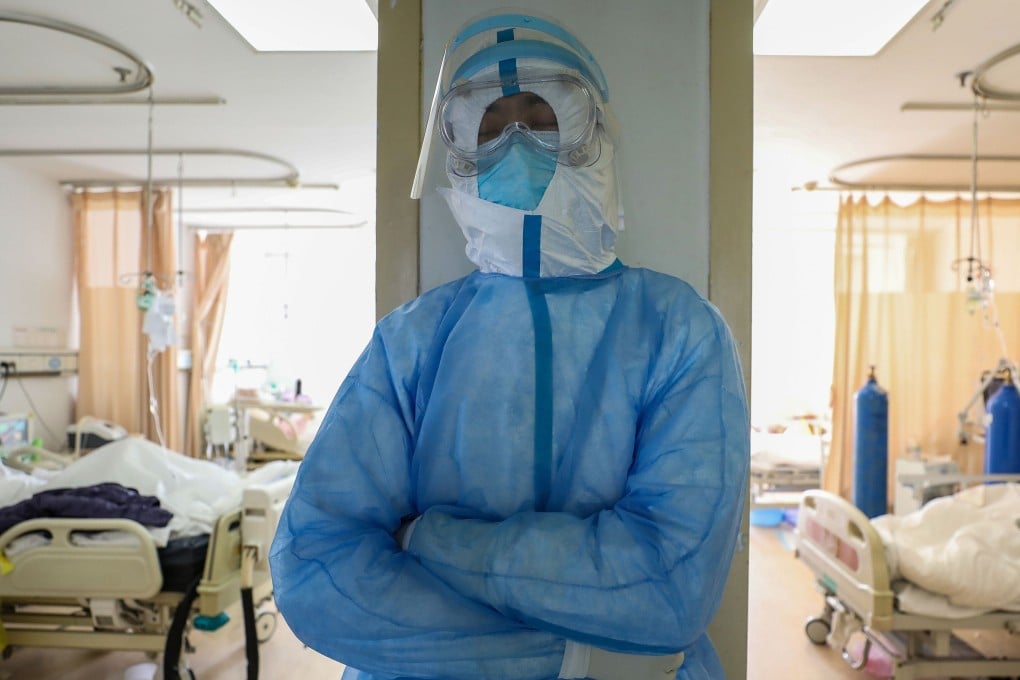
Frontline medical staff treating Covid-19 patients in China and who are experiencing insomnia face long-term health risks, researchers warn.
More than a third of medical staff who responded to the coronavirus pandemic during its peak in China, and who took part in the research survey, suffered from sleeplessness, according to the study, published in Frontiers in Psychiatry. The health care workers who regularly lost good sleep were also more likely to feel depressed, anxious and have stress-based trauma, according to the paper.
“Typically, stress-related insomnia is transient and persists for only a few days,” said Dr Bin Zhang, a professor at Southern Medical University in Guangzhou, China, and co-author of the paper.
Advertisement
“But if the Covid-19 outbreak continues, the insomnia may gradually become chronic insomnia,” he added.
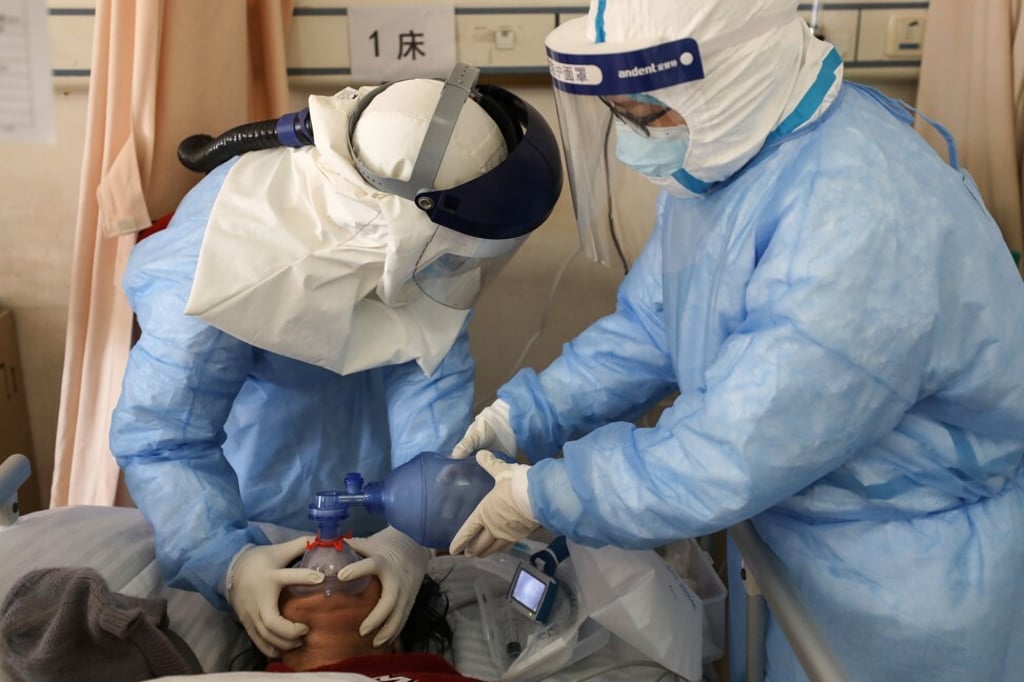
Advertisement
The research was conducted between January 29 and February 3 during the peak of the epidemic in China. To date, more than 83,800 Covid-19 cases have been confirmed in China, with more than 4,630 deaths.
Advertisement
Select Voice
Select Speed
1.00x