Advances in treatment for chronic myelogenous leukaemia
There are more chronic myelogenous leukaemia (CML) sufferers in Hong Kong than ever. But that's a good thing because it means patients are living longer, according to experts.
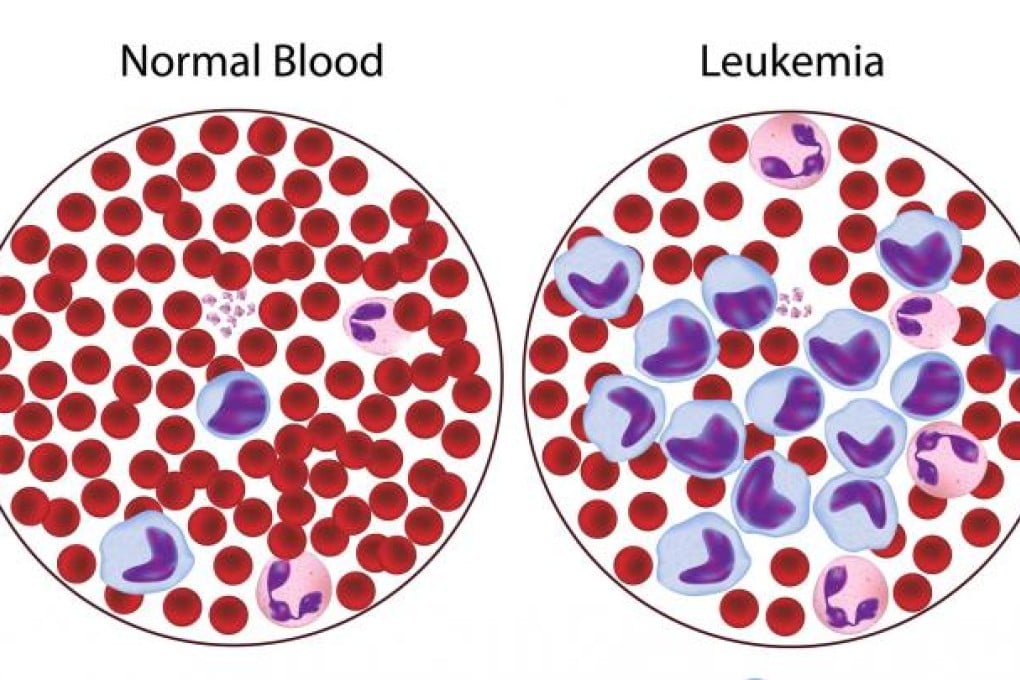
There are more chronic myelogenous leukaemia (CML) sufferers in Hong Kong than ever. But that's a good thing because it means patients are living longer, according to experts.
Once an almost inevitable death sentence, the blood cell cancer has transformed into a nearly always treatable condition in the past decade or so, thanks to targeted drugs known as tyrosine kinase inhibitors (TKIs).
"The prognosis [for CML patients] is now very good," says Dr Herman Liu Sung-yu, a specialist in haematology and haematological oncology. "So we've seen a cumulative increase in patients."
The incidence of CML in Hong Kong is about 0.8 to 1 per 100,000 people, says Liu. About 50 to 70 new cases are diagnosed each year.
CML - one of five types of leukaemia - can occur at any age, but it most commonly affects middle-aged and older people.
Tyrosine kinases are proteins on leukaemia cells that act as on-off switches. TKIs shut down these proteins, in particular a mutant gene known as BCR-ABL, which causes the disease to flourish.