Advertisement
Coronavirus: is China’s rigorous home disinfection prudent disease control, falsely reassuring or overkill?
- Emphasising deep cleaning aligns with Beijing’s persistent view the virus can spread from surfaces, and may originally have been imported into Wuhan on goods
- Experts say better ventilation and air circulation, as well wearing masks, would better prevent the spread of Covid-19
6-MIN READ6-MIN
46
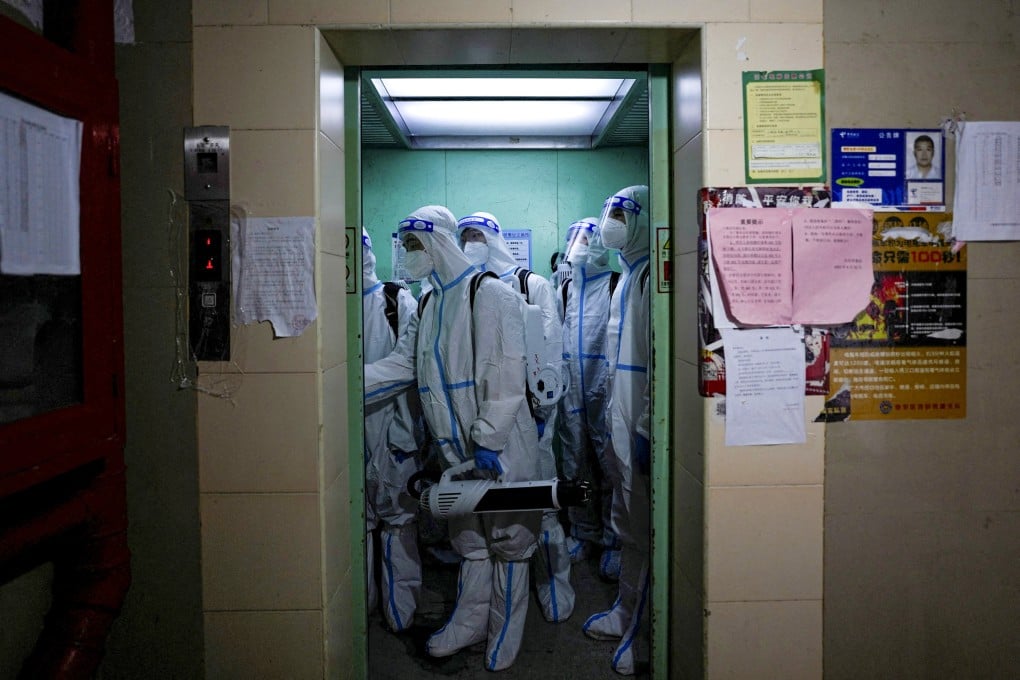
Under China’s tough Covid-19 response, testing positive means not only being taken away for treatment or isolation instead of resting at home, it also means returning home to find everything from the refrigerator to quilts, thoroughly sprayed with disinfectant.
Residents of Shanghai, Jiangsu and Jilin complained online they had found their homes wrecked with disinfectants – in some cases disinfection occurred without the homeowners’ consent.
And last week, the government of Dandong on the border with North Korea, a country now battling an “explosive” outbreak, told residents their homes must undergo deep disinfection before they return from isolation for Covid-19, with or without their consent.
Advertisement
The floor, walls, chairs and tables, toys, cooking pots and dishes, clothes and electronic appliances would be disinfected, a government statement said.
Bedsheets, clothes and pillowcases could be disinfected first and returned to the patient or treated as medical waste, the statement said. Unopened food in the refrigerator may be disinfected and retained, while products that have been opened must be treated as medical waste.
Advertisement
In other words, it is a textbook “terminal disinfection” procedure to thoroughly remove pathogens from an environment, just as a hospital ward does between patients.
Advertisement
Select Voice
Select Speed
1.00x