Advertisement
Doctors on front line of China’s battle with coronavirus tell of race to respond to onset of new disease
- One doctor in Wuhan describes the emotional toll of trying to care for Covid-19 patients and warns that the most serious cases are still struggling to make it
- Medical staff had to learn on the job when treating the previously unknown disease, which may have cost some patients their lives
3-MIN READ3-MIN
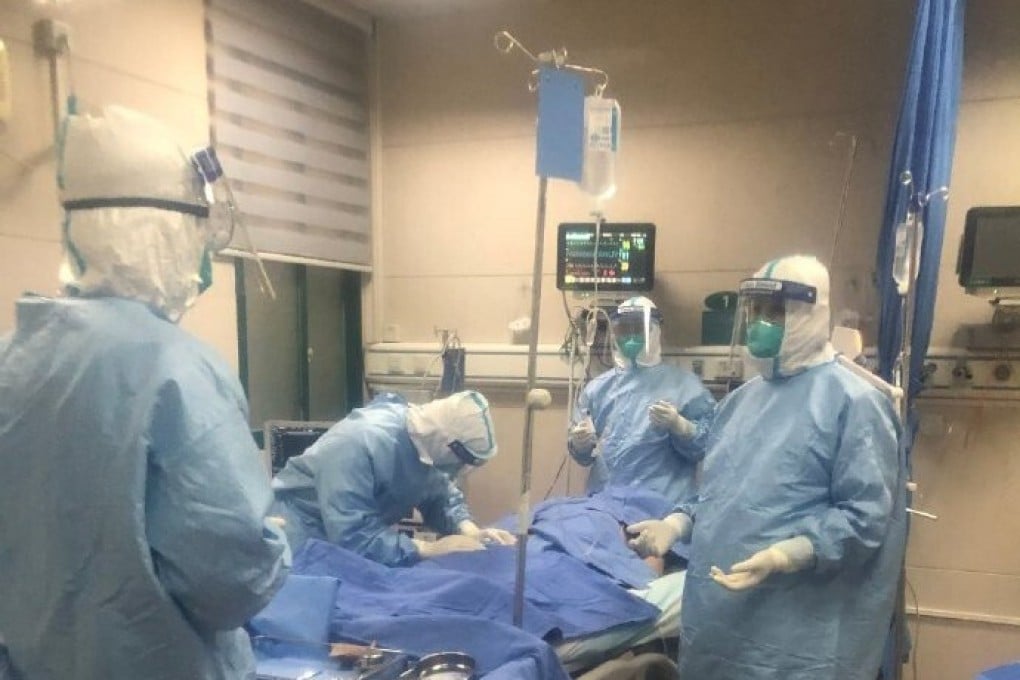
As a veteran critical care doctor, Peng Zhiyong from Zhongnan Hospital in Wuhan has seen his fair share of deaths, especially when dealing with the deadly Sars outbreak in 2003 and bird flu in 2016.
But he admits that sometimes while fighting the Covid-19 outbreak he broke down in tears, particularly when his department had to turn away critically ill patients because of a shortage of beds or when patients died despite medical workers’ best efforts to save them.
“I couldn’t calm down in the face of death, but I just had to pull together to do my job,” said Peng.
Advertisement
China is slowly recovering from the outbreak of the new coronavirus which causes the disease, but doctors like Peng are still battling to save some of their most seriously ill patients.
At the start of the week 600 cases in the country were still listed as severe, down from a peak of 12,000 in mid-February.
Advertisement
Advertisement
Select Voice
Select Speed
1.00x