Hong Kong hospital crisis: overcapacity, overworked doctors — and peak flu season will make it worse
After bed occupancy rate exceeds 100 per cent on Tuesday, Dr Ko Wing-man says urgent measures like suspending non-emergency services to be weighed
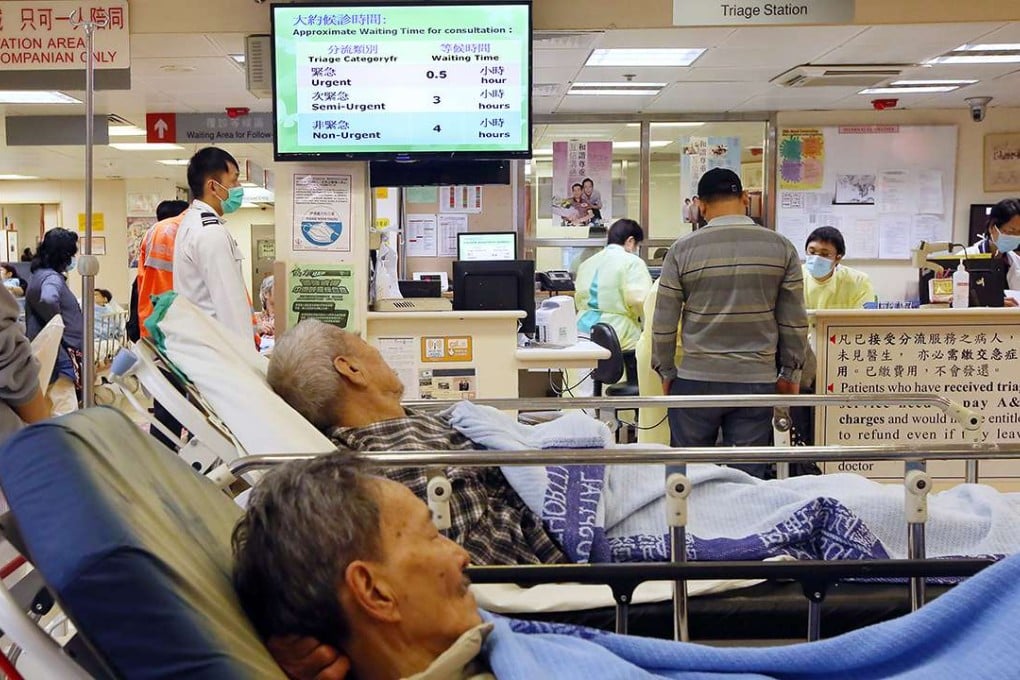
Hong Kong’s public hospitals have been stretched to breaking point by a surge in the number of patients seeking treatment for flu and chronic diseases during persistent cold weather.
The “unprecedented” problem has now spilled over from emergency units and medical wards to departments like orthopaedics and surgery, the Post has learnt.
READ MORE: An eternal wait: Some Hong Kong patients have to wait more than 20 hours to get into hospital amid overcrowding
The occupancy rate on all medical wards in 16 public hospitals has consistently been around 110 per cent, with some as high as 130, meaning temporary beds have even filled up all spaces in corridors.
Some patients complained of waiting for days in observation units before they could be moved into a room.
At accident and emergency units, patients classified as non-urgent were made to wait for as long as 24 hours before they were seen by doctors, with over 7,000 patients attending the units daily over the past week, compared with the average of 6,000.