Explainer: a brief history of TB in Hong Kong, as experts fear global comeback of the disease
While the global fight against tuberculosis is being won, Hong Kong still sees many new cases each year, and overseas experts have urged greater action against it
Tuberculosis, or TB, was once one of the most deadly diseases in Hong Kong and other Asian cities, and still leaves a lingering fear among older generations.
Many traditional television dramas featuring the period when the “white plague” was a threat often had scenes of patients coughing up blood, which signified a virtual death sentence.
A breakthrough came in the 1950s when big strides were made in the battle against the disease. First, a cure was discovered; second, the colonial government started a partially effective vaccination programme for newborns; and third, hygiene in Hong Kong improved dramatically. These measures helped stop the spread of the global threat, with public attention and media coverage fading away over time.
Despite the improvements, the disease never really left the city. Outbreaks still happen from time to time, with more than 4,412 people becoming infected and about 155 dying every year. About 10 school outbreaks have been recorded every year, according to the Department of Health.
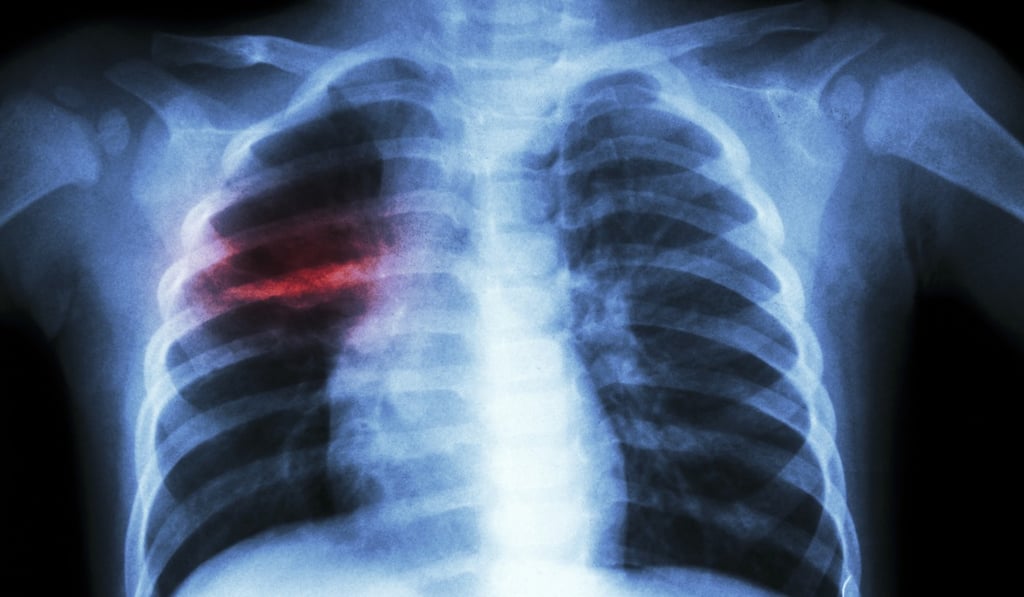
In recent years, experts have expressed fears of a global comeback of the disease, complicated by the fact that there has been a rise in the number of drug-resistant cases, frequent travels between disease hotspots and very crowded and cramped living environments.
Eight cases of tuberculosis confirmed at Hong Kong secondary school
A recent outbreak in a Sha Tin secondary school, Kiangsu-Chekiang College, that infected eight people has again exposed the risks of the disease and left questions over whether the government is doing enough to prevent it. Overseas experts have urged the Hong Kong government to show more commitment in responding to the World Health Organisation’s strategy to eliminate TB by 2035.