Breakthrough HKUST-led research on mapping of HIV weak spots paves way for vaccine
Scientists processed data from nearly 2,000 patients globally to map regions of a crucial protein on the virus surface
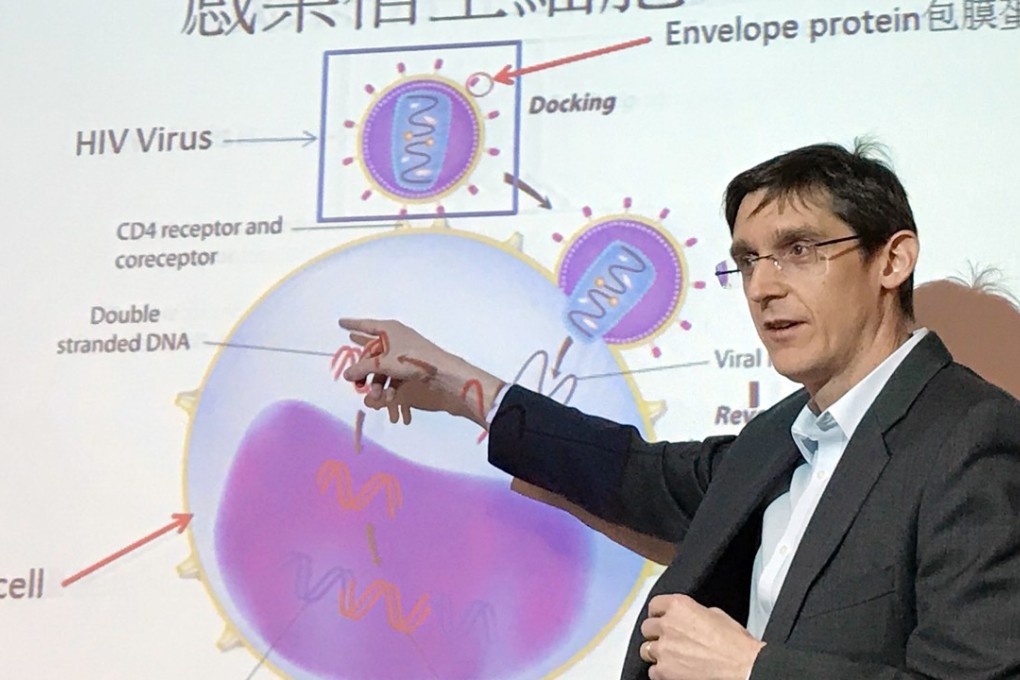
Data scientists have discovered a way to map weak spots in HIV, potentially paving the way for researchers to design a vaccine.
An international team of scientists led by the Hong Kong University of Science and Technology processed data from 1,918 HIV-infected patients globally to map the protein protrusions on the virus’ surface that predict how it mutates and its ability to replicate.
HIV, which attacks the immune system, is hard to tackle because it rapidly mutates and changes its appearance to evade antibodies that a person’s immune system produces to fight off the virus.

By using a computational framework they developed, the scientists were able for the first time to identify a fitness landscape – a map that shows how it mutates, and its ability to assemble and replicate itself in the body.
Hong Kong government cuts cash for HIV prevention, just as infections set to surge
“The fitness landscape of the HIV virus is currently not well understood … what we can do with our landscape is that we can predict for any mutation, whether it’s fit or not,” said Matthew McKay, associate professor in HKUST’s department of electronic and computer engineering.