Advertisement
Baby Yu-yan: liver donor comes forward to give Hong Kong toddler new hope
- Parents announce family friend has agreed to donate his liver to help sick infant
- Child, 23 months old, went into cardiac arrest after liver surgery
Reading Time:2 minutes
Why you can trust SCMP
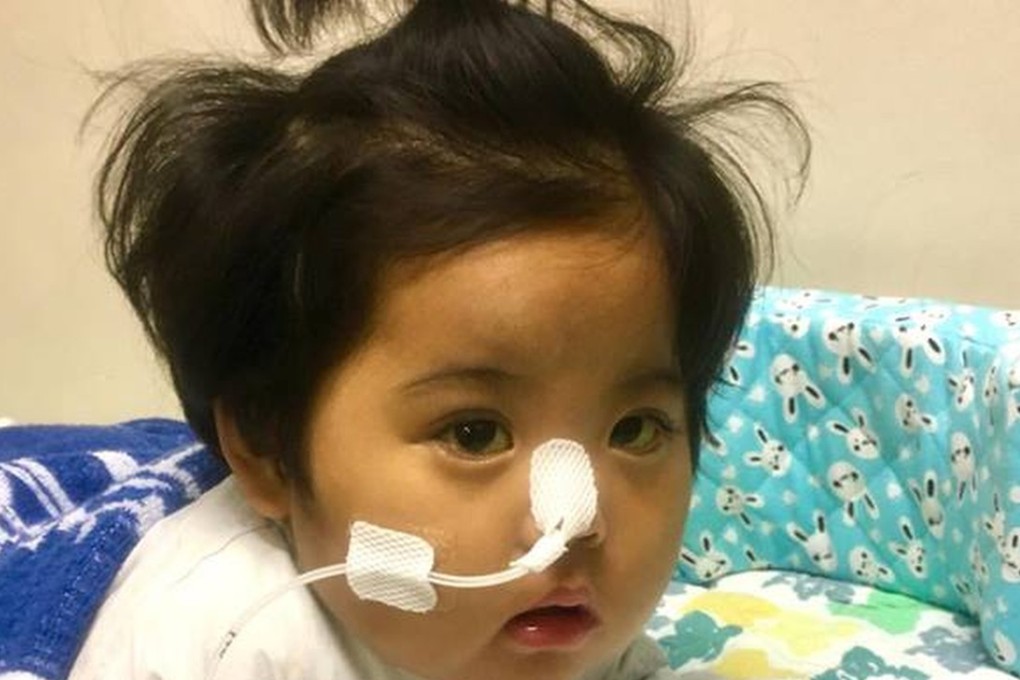
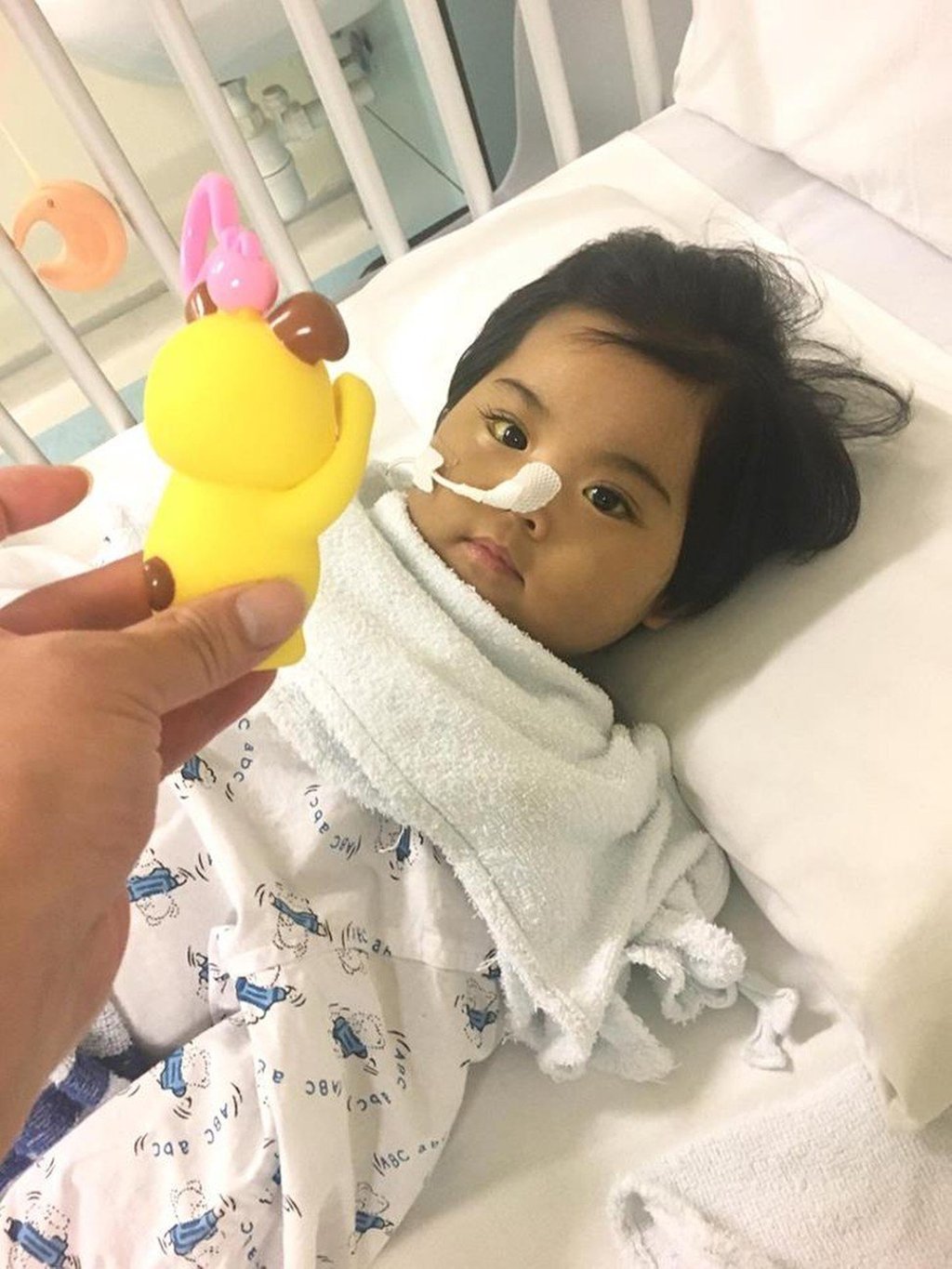
There is new hope for the 23-month-old Hong Kong baby who suffered a cardiac arrest following liver surgery at a public hospital, with a suitable organ donor being identified.
The family shared the news in a post on a Facebook page dedicated to the recovery of the baby, called Yu-yan, on Sunday night, saying that“a friend” was willing to be a donor.
“He is a long-time friend of ours,” the baby’s father confirmed to the Post on Monday.
Advertisement
“We are very much grateful for his selfless love,” said the father, who preferred to be identified only as “Yu-yan’s father”.
The father revealed doctors would need to cut away as much as a third of his friend’s liver for the transplant.
Advertisement
Advertisement
Select Voice
Select Speed
1.00x