Malaysia’s coronavirus vaccination drive offers hope, but burnt-out doctors are quitting
- Malaysia on Wednesday saw a record number of new Covid-19 cases, with a peak expected in September, despite its ongoing vaccine roll-out
- Exhausted medical workers blame Muhyiddin Yassin’s government for mismanagement, and compare the situation to India’s surge in May
Last week, however, Health Ministry secretary general Noor Hisham Abdullah said hospitalisations and intensive care admissions in densely populated places such as Kuala Lumpur and Putrajaya were gradually decreasing following the vaccination drive.
The Tengku Ampuan Rahimah Hospital in Klang, which was earlier reported to be drastically over capacity, has seen admission rates drop by 50 per cent since last week, an official said on Tuesday.
But with the daily caseload remaining at record levels, doctors say they are at their wit’s end and see no end in sight to the long hours and having to make daily decisions on which patients live or die.
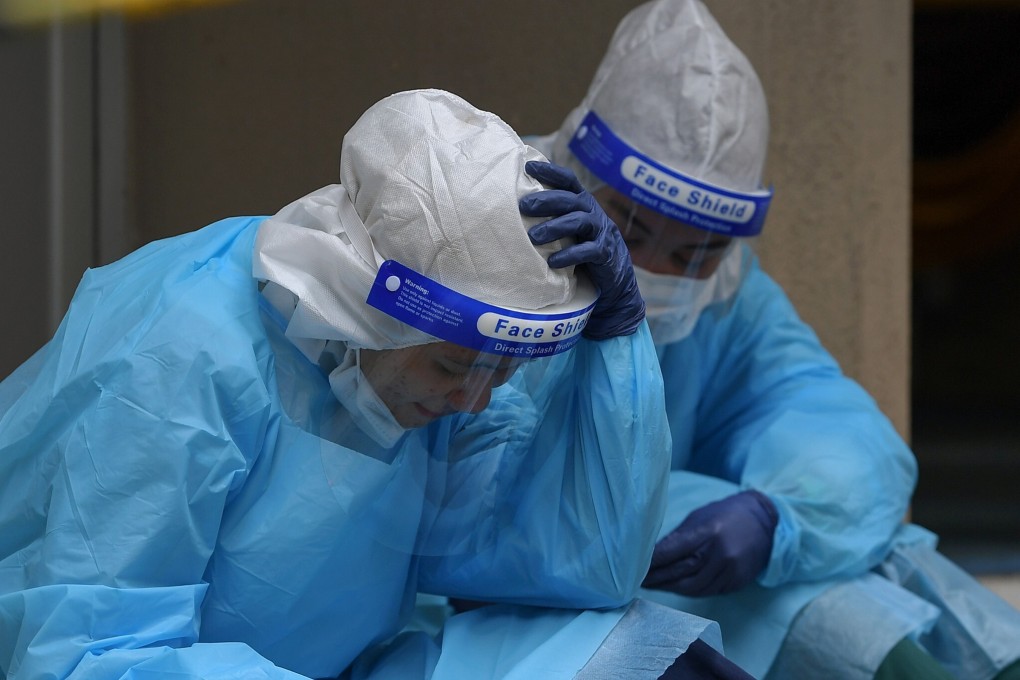
Dr Raja, who did not want to give her real name or the hospital she works at, told This Week in Asia that the emotional toll of the situation had left many of them “beyond exhausted mentally and physically”.