Afghanistan’s running out of medicine, oxygen in hospitals with health sector facing ‘dark future’
- A survey of 940 public health facilities after the Taliban took power found two-thirds are short of medicine and can’t pay staff
- It also found a lack of oxygen as well as PPE for doctors, and medical workers that had not received a salary for the past four months
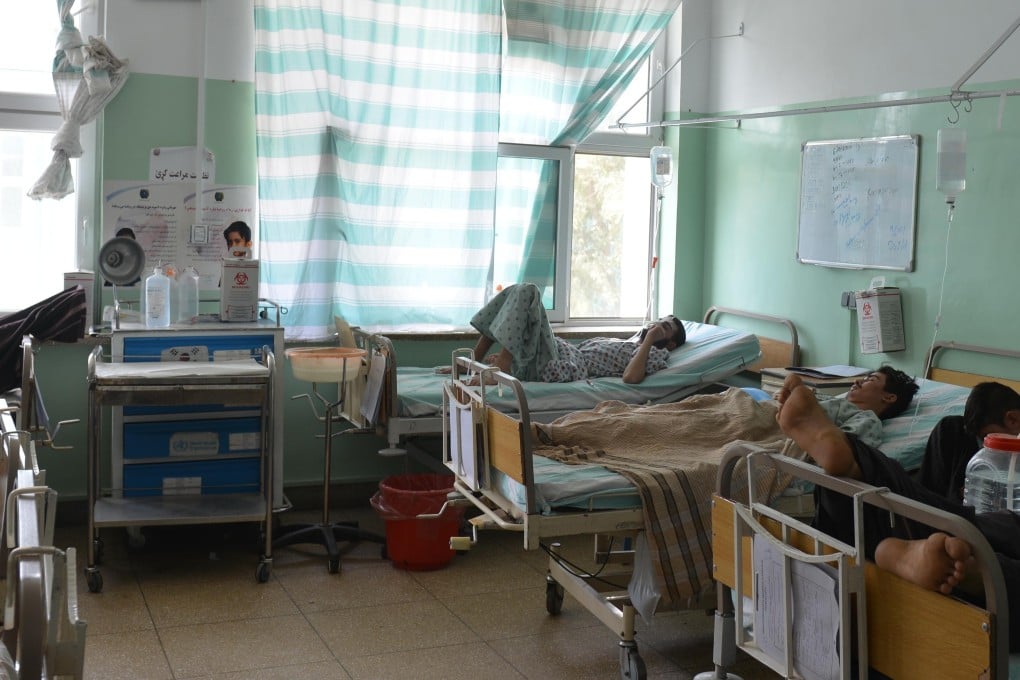
Close to two-thirds of public health facilities in Afghanistan are facing a shortage of medicine, while 63 per cent of their staff have not been paid for the past four months, a new survey has revealed.
“The lack of medicine, and the unpaid salaries, are alarming findings, and it clearly highlights that the future of the health sector is dark,” the group’s head of research Ezatullah Adib told This Week In Asia. “This survey was designed and implemented to derive a clear picture of the state of the health system, highlight its major deficiencies and make recommendations to avoid its collapse.”
Although Afghanistan’s understaffed and ill-equipped health system is reliant on donations, many agencies stopped supporting the country’s facilities soon after the Taliban’s return to power.
According to the World Health Organization, only 3 per cent of health facilities are fully operational, and two-thirds do not have the necessary basic care. On top of this, the World Bank’s US$600 million Sehatmandi project – which was the main source of funding for more than 65 per cent of such facilities in Afghanistan – has been suspended.