Indonesia’s health scheme dwarfs Obamacare. But there is a problem
Jakarta has gained much political capital by rolling out the world’s biggest universal health insurance programme. There’s just one snag: paying for it

When Dr Selvy Anggeraini took over as the head of one of Jakarta’s busier government health clinics, she had a budget of 1 billion rupiah (US$72,500) to treat the 350 or so patients that came daily to seek care from one of her 14 doctors. Four years later, after the introduction of a generous universal health insurance programme, her caseload has doubled, even though her budget has barely moved.
“The care is mostly free so now more people come,” says Anggeraini, whose district – home to 350,000 – spans some of the wealthier suburbs in the south to the working class districts in the north. And while Anggeraini is adamant the clinic cuts no corners to make ends meet, she allows that the clinic is stretched thin. “We have to make the same budget go further. It’s not enough.”
Indonesia is one year away from completing a five-year roll out of what is already the world’s biggest universal health insurance programme – one that makes Obamacare look practically third world in its ambitions. So far 185 million – about three quarters of the population – have signed up, availing themselves of generous benefits that until recently were unthinkable for most here.
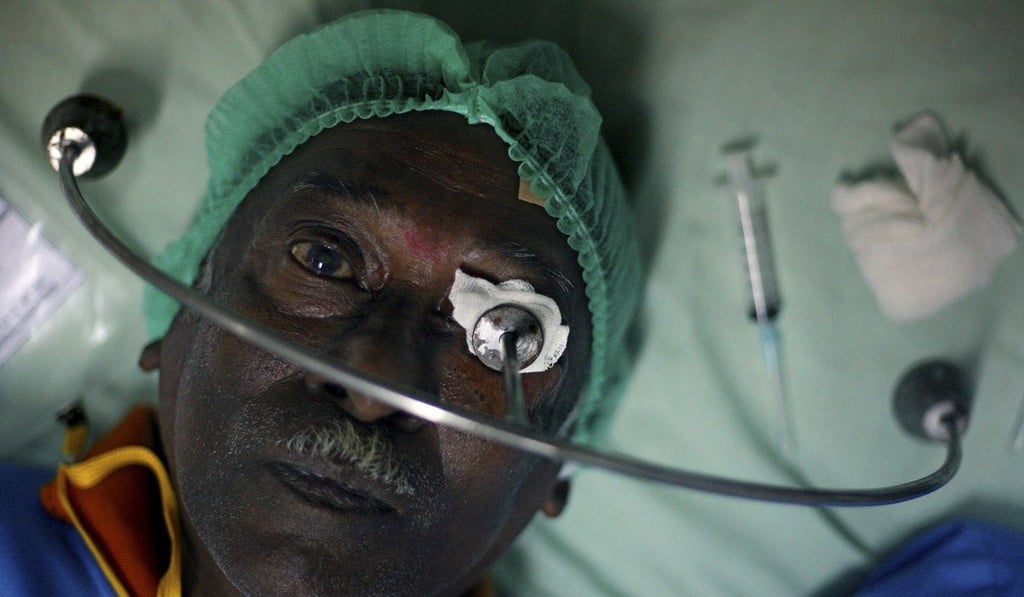
It’s a far cry from what was available before the insurance. The poor then either stayed sick or went into debt to pay for treatment, Anggeraini says. Most of her patients then would refuse referrals to specialists because they couldn’t pay.
Why are ethnic Chinese still being denied land in Indonesia?
“It was heart breaking,” Anggeraini recalls. “We didn’t feel like we were making people better.”