Coronavirus models made governments take action, but how useful are they really?
- Infectious disease modelling helped convince countries to make extraordinary moves in a bid to curb the spread of the Covid-19 pandemic
- But how these models work is little understood by either policymakers or the public, and there is growing scepticism about some of their predictions
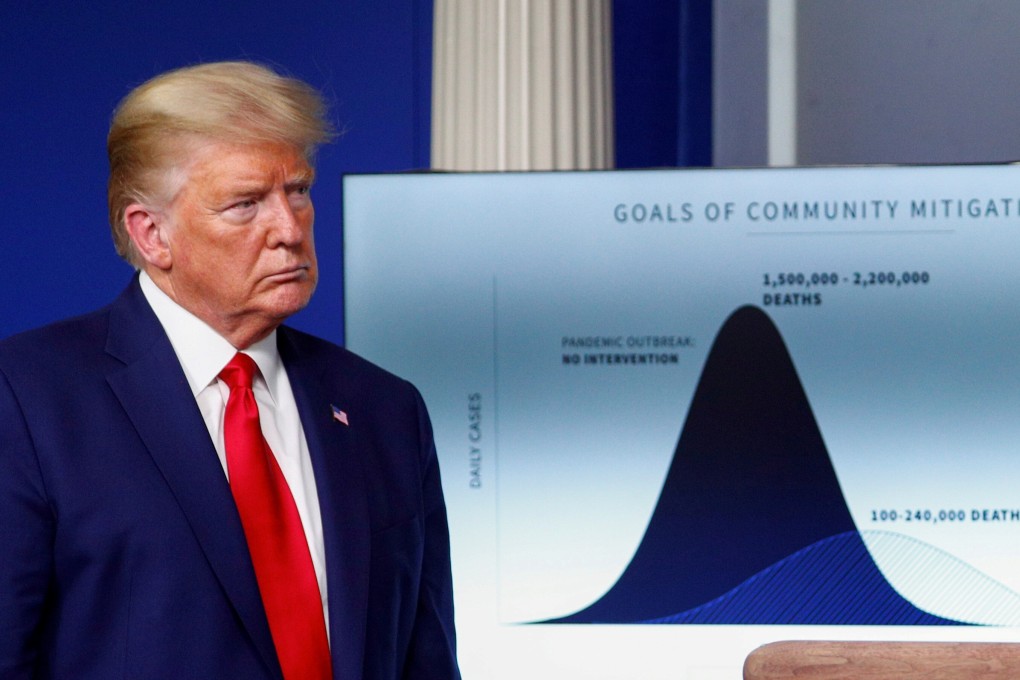
The dramatic policy U-turn was a striking, but far from isolated, example of the extraordinary influence that computer models have had on how governments around the world are responding to the pandemic, which has resulted in more than 2.6 million confirmed infections and about 190,000 deaths so far.

Although models have been part of the toolkit for fighting infectious disease since the 1800s, their enormous impact on policymaking during the pandemic has raised questions about their accuracy, limitations and risks – including whether authoritative-sounding calculations may ironically blind governments to their full range of options when tackling a crisis with ramifications for every aspect of society.
When modellers made the decision to look at certain public health interventions over others, for example, it could lead governments to formulate responses that might be less effective, said Yaneer Bar-Yam, president of the New England Complex Systems Institute and co-author of a paper critiquing the Imperial College model.