
The new diabetes breakthroughs that could change lives, and a type 1 sufferer on what it would mean to him
- Recent breakthroughs are allowing doctors to understand type 1 diabetes better than ever, and pharmaceutical companies are betting big on a cure
- Sufferer Simon O’Reilly talks about his experience with the disease and the difference these breakthroughs could make to him
Today, 425 million people live with diabetes worldwide – about 1 in every 11 adults – according to the International Diabetes Federation, and that number is set to balloon.
By 2045, the number is expected to be almost 630 million, a rise of close to 50 per cent and roughly six times the 108 million estimated by the World Health Organisation to have diabetes in 1980. And every year, the average age for being diagnosed with diabetes gets younger.
These numbers are daunting, not just for people living with diabetes, but for health care professionals struggling to treat the condition, which 46 per cent of sufferers don’t even know they have.
It can be especially discouraging for suffers of the rarer, more mysterious, type one diabetes (T1D), previously called “juvenile diabetes”, since most people are diagnosed in their youth, at an average age of 14 years.
But recent breakthroughs and lucrative new funding streams for research are giving doctors and T1D diabetics hope which, until recently, had been in short supply.
Simon O’Reilly is a production editor for SCMP.com and has been living with T1D for 23 years. He describes how he first learned of his affliction.
“I had a swelling on my neck that grew really quickly over two weeks. I lost a lot of weight – almost 30kg [66 pounds] – and was getting pins and needles in my left arm. My eyesight would occasionally blur for a minute or two. I was also urinating way more than normal,” he remembers.
“After my neck was operated on, a doctor came and said I was diabetic and took my cup of tea away. That was the last time I had sugar in my tea or coffee. Then I was taught how to inject myself [with insulin] and test my blood.”
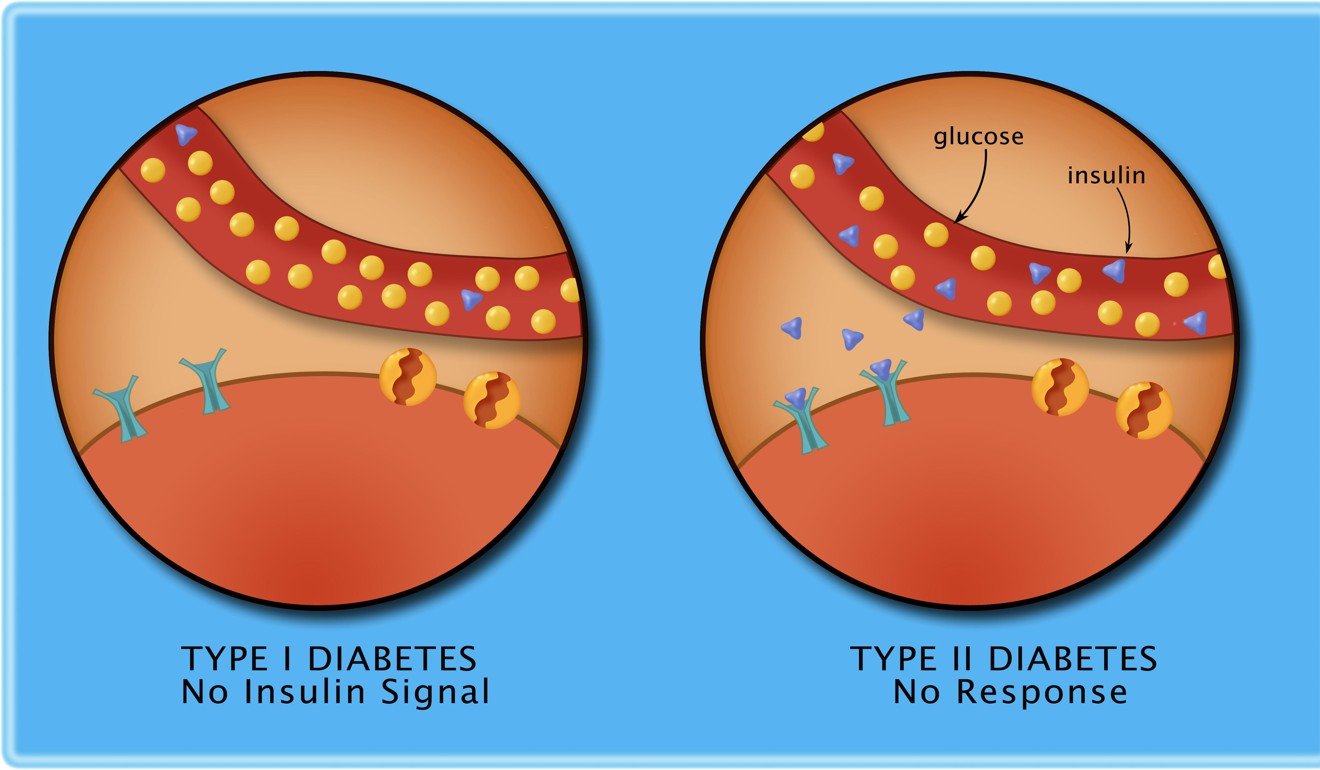
If you inject insulin, but fail to eat enough, “the brain uses a huge amount of fuel and starts to shut down without it,” O’Reilly explains. “If no extra sugar is introduced, your condition deteriorates fairly quickly to loss of consciousness, coma and death.”
Conversely, too much glucose and not enough insulin – hyperglycaemia – leaves the diabetic feeling sick. While it may feel less severe in the short term, it causes much of the long-term damage diabetics suffer. If left untreated for more than a day or two, it can even be fatal.
“Managing type 1 diabetes is all about balance,” says O’Reilly, whose daily routine includes four injections.
The hardest thing is to come to terms with your own mortality, loss of stamina and losing the freedom to eat what you want
Recent breakthroughs allow doctors and scientists to understand T1D better than ever. Pharmaceutical companies are starting to bet big on a long-elusive cure.
The first step to developing more successful T1D treatments and a cure is to discover what causes the disease. That is the goal of researchers at the University of California San Diego who, in August, received grants of US$9 million to fund two separate multi-institutional programmes using stem cells and the gene-editing Crispr technology to determine what happens on a cellular level.
Studies like these are so advanced, they sound like science fiction. For example, information gleaned from the UC San Diego research will be used for tests on “human organoids” – miniaturised 3D versions of human organs.
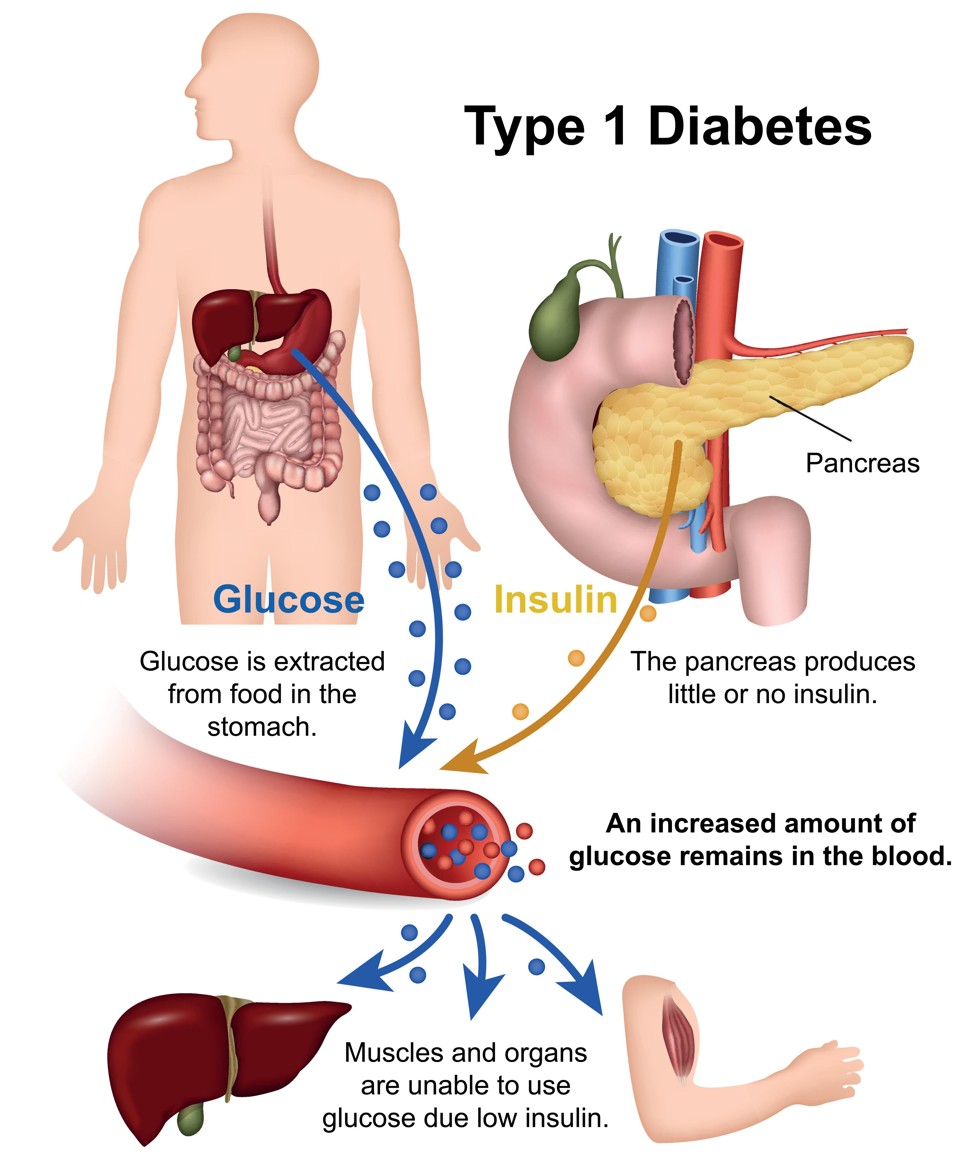
Other recent findings focus on treatment and improving T1D patients’ lives. Scientists conducting a trial run with mice at Scripps Research Institute in California discovered what is likely the earliest possible biological marker of T1D. If they can replicate this in humans, doctors should be able to determine which patients will develop the disease years earlier, radically adjusting treatment.
“Discovery paves the way for earlier detection of type 1 disease: an early diagnosis … and the ability to monitor beta cell destruction in real time will allow a series of new therapeutic interventions aimed at preventing type 1 diabetes,” says the group’s paper.
For a condition such as T1D, early diagnosis is key. Similar to the research at Scripps, a group of European scientists funded by the JDRF (formerly the Juvenile Diabetes Research Foundation) claim to have developed a test that can determine T1D in babies as young as three months old.
Delaying the progression of the disease is an essential and impactful step toward the prevention, and ultimately a cure for type one
Early treatment of the most vulnerable patients would improve quality of life from earlier on, a head start O’Reilly would have appreciated.
“The list of side effects is long. Heart and blood vessel disease, kidney damage, foot damage, skin and mouth conditions, and reduced life expectancy … and T1D can lead to gangrene, loss of limbs and much more,” he says.
While recent work deals with diagnosis, other breakthroughs hold promise for delaying the disease’s onset entirely. Enter Teplizumab, a drug that can postpone T1D for up to two years.
The drug was unveiled at the American Diabetes Association’s 79th Scientific Sessions in June by TrialNet, an international research network dedicated to developing treatments and a cure. Speaking at that presentation, Aaron Kowalski, president and CEO of JDRF, said: “Delaying the progression of the disease is an essential and impactful step toward the prevention, and ultimately a cure for type one.”

Any real progress towards a cure will necessarily involve beta cells, which measure the body’s glucose levels and produce insulin accordingly. Normally beta cells are found in the pancreas, but in T1D patients, the pancreas does not make any or enough insulin because the body’s own immune system, for reasons still unknown, attacks its beta cells.
Researchers at Harvard University have managed to create beta cells in the lab. In 2020, Semma Therapeutics – started by the Harvard researcher behind the development of such beta cells – will use its US$100 million in venture funding to test the lab-made beta cells in humans.
Huge strides have also been made in the development of the holy grail of T1D treatment: the artificial pancreas.
There is technology that effectively outsources the pancreas’ job, monitoring blood glucose levels and using pumps to supply the blood with insulin. But even the best devices need constant management. The dream is to create a device that, like a pacemaker, mimics the whole pancreatic system without oversight. Professor Roman Hovorka of the UK’s University of Cambridge is working on this type of device, which is now in advanced human trials.
Gout explained: its symptoms, and foods and drinks to avoid
To gauge the excitement around the future of T1D treatment, and the potential for a cure, you need only look at the money. In September, Vertex Pharmaceuticals announced that it would acquire Semma Therapeutics for US$950 million. Treatments that Semma is developing, if effective, are conservatively expected to earn the company more than US$10 billion a year.
The potential of new drugs has normally cautious researchers talking about a possible T1D cure in terms of not if, but when – raising patients’ hopes.
“The hardest thing is to come to terms with your own mortality, loss of stamina and losing the freedom to eat what you want,” O’Reilly says. “A cure would return my independence and give me back control of my life.”

