
Explainer | How diabetes can trigger vision loss and blindness; 11 signs of diabetic retinopathy, and how to treat or prevent it
- High blood sugar caused by diabetes damages blood vessels in the body, including the eyes – but there may be no symptoms early on
- Early detection and treatment can halt or slow vision loss; here are 11 signs telling you to see an eye doctor
Not all diabetics know that their eyes are in the disease’s cross hairs, too.
Damage to blood vessels in the retina can cause a condition known as diabetic retinopathy. At worst, it may lead to blindness, warns German ophthalmologist Dr Ulrich Kellner.
While it can’t be cured, proper treatment can prevent, delay or reduce vision loss.
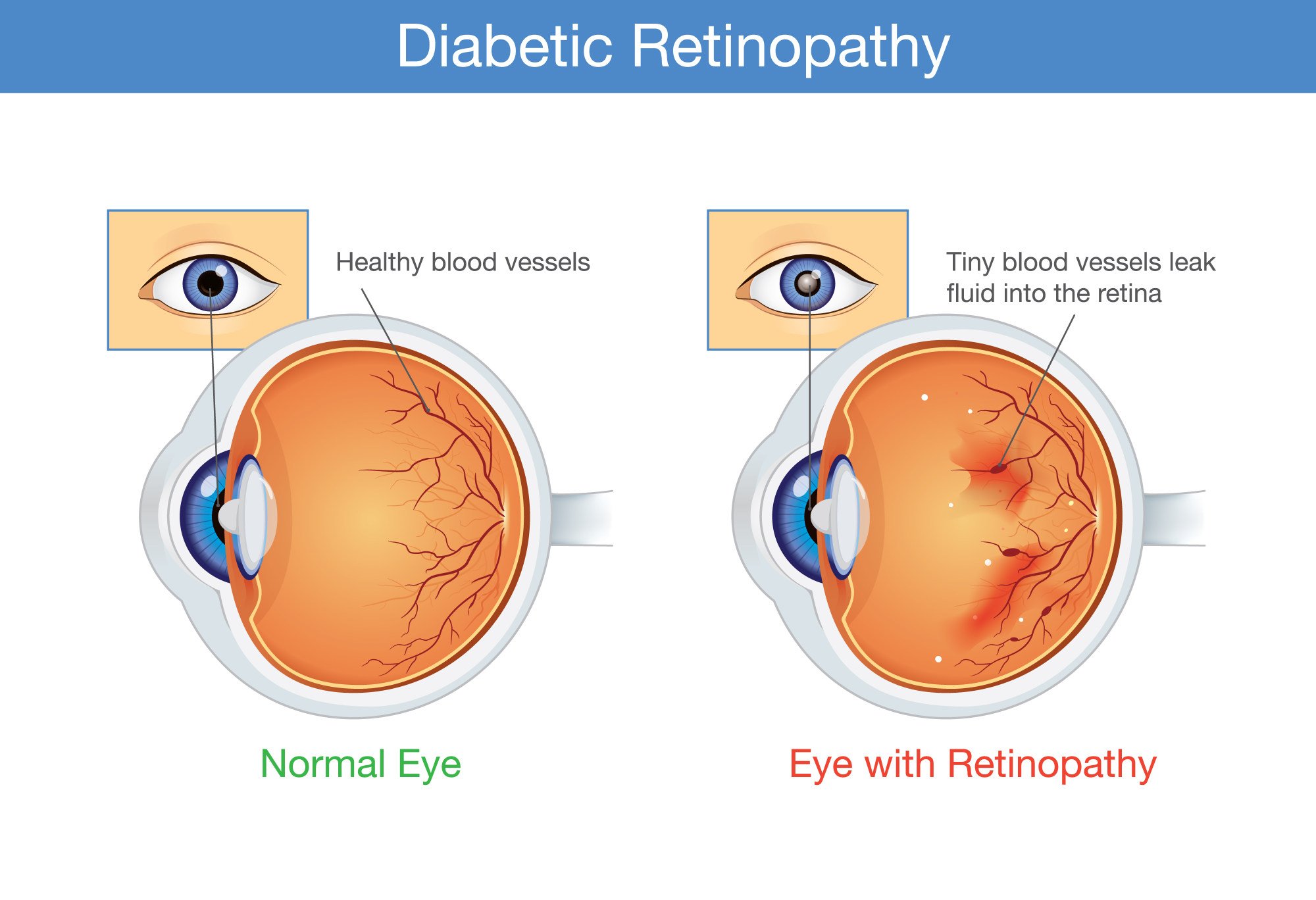
The retina is the light-sensitive layer of tissue at the back of your eye. Its photoreceptor cells convert light that enters the eye into electrical signals that the optic nerve sends to the brain, forming a visual image.
“First the tiny blood vessels [that nourish the retina] become partially blocked, and then the larger ones,” explains Kellner. This can cause them to leak fluid and blood into the retina.
From riding roller-coaster to myopia, causes and risks of a detached retina
In a later stage, the eye tries to make up for its oxygen deficit by growing new blood vessels. But they’re fragile and can leak into the vitreous, the clear, gel-like fluid that fills the centre of the eye.
The abnormal blood vessels also stimulate growth of scar tissue, which eventually contracts. This can pull on the retina and detach it.
“Both of these things can dramatically worsen vision,” Kellner says.
In many cases, damaged retinal blood vessels leak fluid into the macula, the round area at the centre of the retina used for sharp central vision. This fluid build-up is called diabetic macular oedema.
Type 2 diabetes is insidious – most affected people don’t know how long they’ve had it
“As the retina gradually thickens, vision becomes progressively blurrier. So it’s harder to read or see clearly enough to drive,” Kellner says.
It’s important to detect diabetic retinopathy early, but it isn’t always easy.
“Type 2 diabetes [formerly known as adult onset diabetes] is insidious – most affected people don’t know how long they’ve had it,” says Kellner, who advises people to get an eye exam soon after a positive diagnosis.
If no problems are found and the patient’s blood sugar levels are under control, another check-up should be done after two years.
“But if blood sugar control is poor, the risk is higher and eye exams should be done more frequently,” Kellner says.
Diabetes and its health risks, from kidney and heart failure to amputations
The situation is different with type 1 diabetes, once known as juvenile diabetes and by far the most frequent type in children and adolescents.
“Their eyes should be examined about five years after the appearance of type 1 diabetes,” Kellner says. “Nothing will happen before then.”
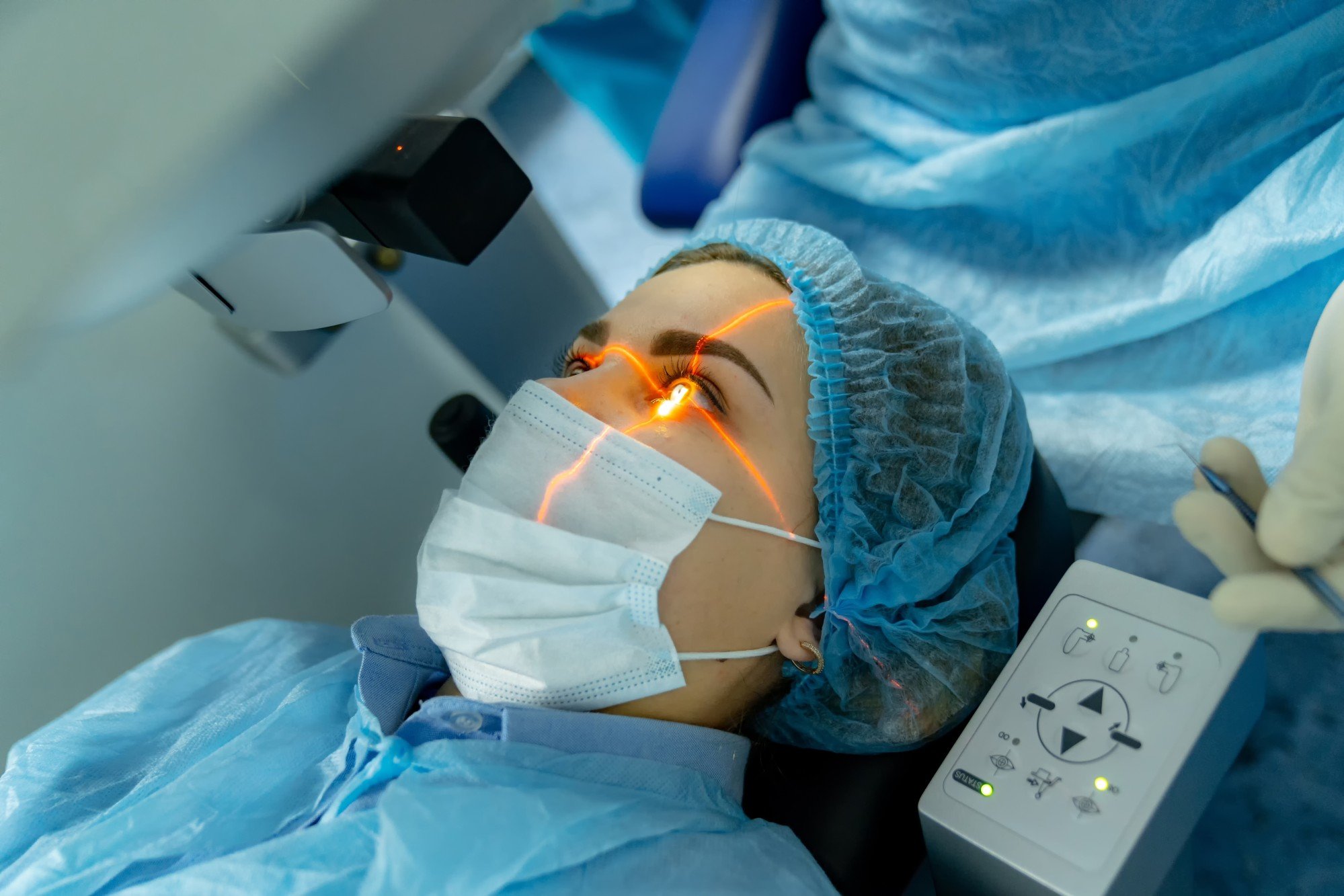
The standard treatment for diabetic retinopathy is laser therapy, according to Kellner. It can stop or slow blood and fluid leakage in the eye, and shrink abnormal blood vessels.
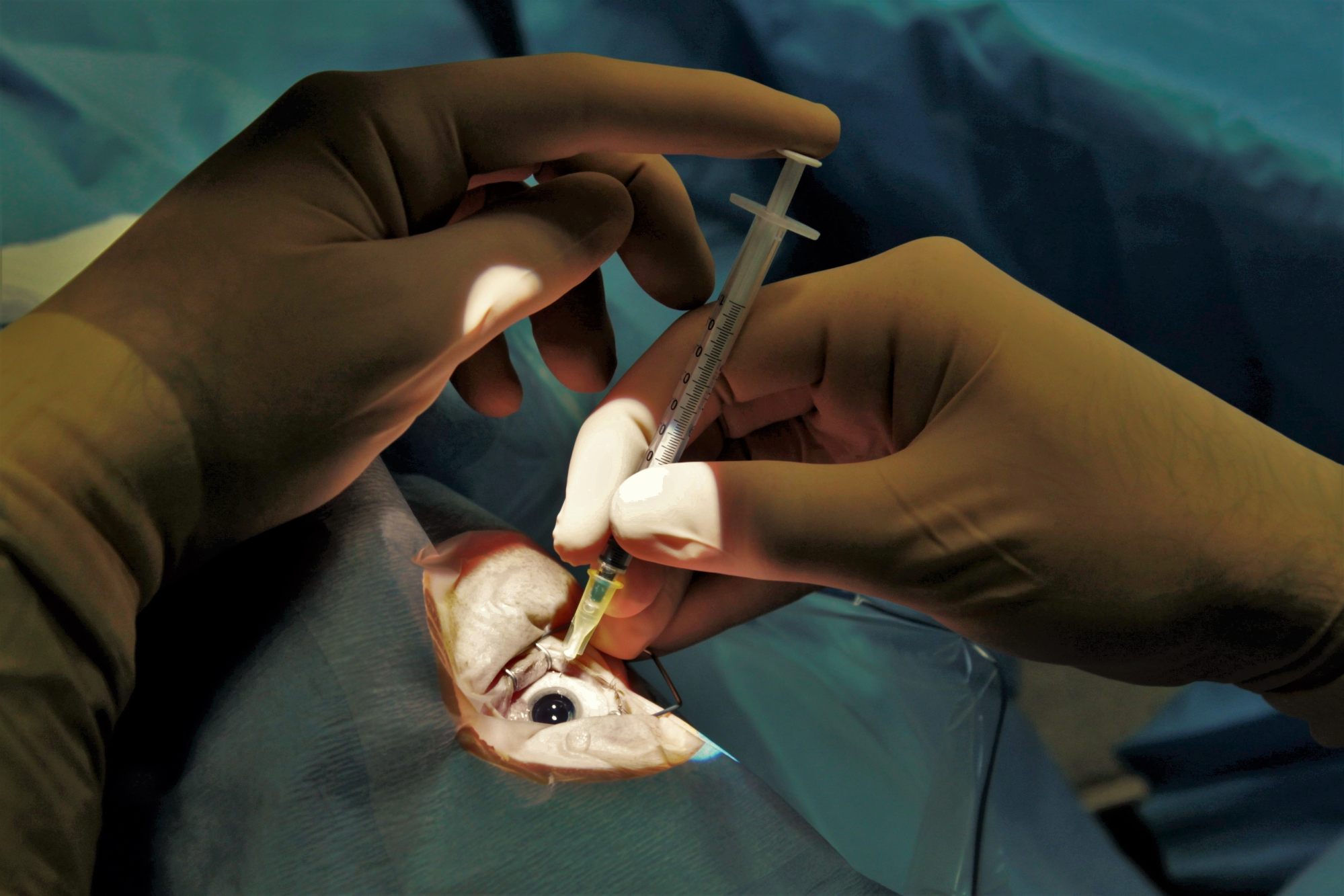
“They seal the blood vessels, preventing further leakage,” explains Kellner. “The fluid build-up recedes, and vision improves.”
While eye injections sound scary, the eye is numbed first and the injections are barely felt. Kellner says the medications have sharply lowered the risk of going blind from diabetic retinopathy.
When to see a doctor
Early detection – and early treatment – can halt or slow vision loss. According to the Mayo Clinic of Rochester, in the US state of Minnesota, you should see your doctor if you have any of these eye-related problems:
-
blurred vision
-
double vision
-
a dark or empty spot in the centre of your vision
-
difficulty reading
-
difficulty seeing well at night
-
droopy eyelid
-
eye pain
-
flashes of light
-
halos around lights
-
objects appear larger or smaller than usual
-
the sudden appearance of spots or “floaters” in your field of vision
Additional reporting by Staff reporter

